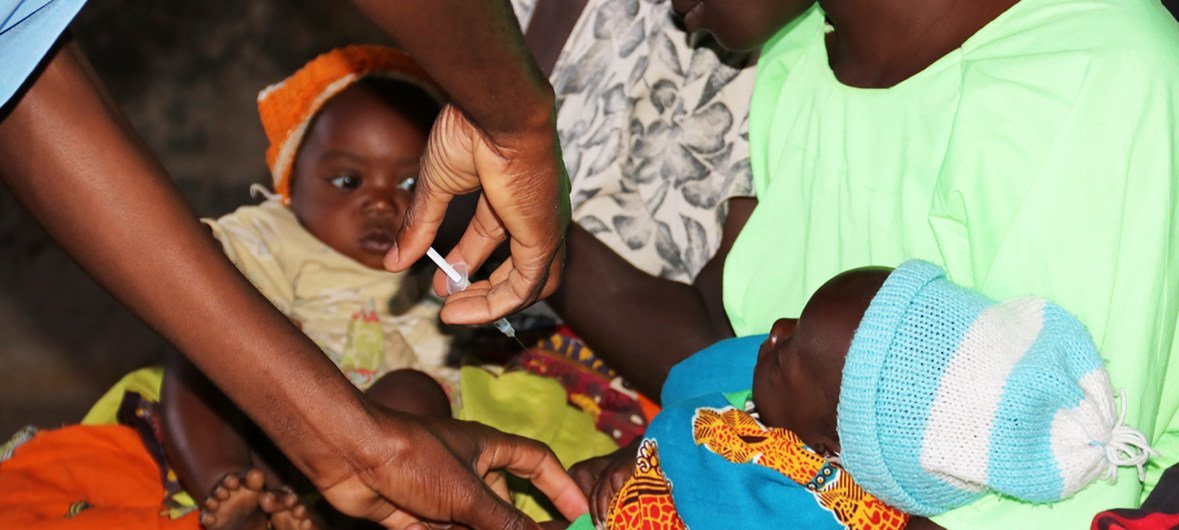
Second malaria vaccine for children is approved by the WHO
According to WHO Director-General Tedros Adhanom Ghebreyesus, two expert panels’ recommendations that the new malaria vaccine be used in children at risk led to the U.N. health agency’s approval of the drug.
“As a researcher on malaria, I used to daydream about the possibility of developing a malaria vaccine that is both secure and efficient. We now have two,” Tedros declared.
The vaccination was authorized by regulatory bodies in Ghana and Burkina Faso earlier this year.
According to John Johnson from Doctors Without Borders, “This is one more tool we will now have, but it won’t replace bed nets and spraying insecticides.” “This is not the malaria vaccine that will end the disease.”
Johnson was not a member of the WHO expert panel that approved the Oxford vaccine.
In a “historic” move to reduce the havoc the mosquito-transmitted disease causes in Africa, which accounts for the majority of the projected 200 million cases and 400,000 deaths worldwide, WHO approved the first malaria vaccine in 2021.
However, the GSK-produced Mosquirix vaccine only offers approximately 30% protection, needs four doses, and wears off after a few months. However, according to WHO experts, there is no evidence to date demonstrating which vaccination, created by GSK or Oxford, is more successful.
The Bill & Melinda Gates Foundation, one of the GSK vaccine’s biggest backers, stepped back last year from financially supporting Mosquirix’s rollout, saying it was less effective than officials would like and that funding would be better used elsewhere.
The main distinction between these two vaccinations is availability, according to Johnson, who noted that just a few of nations are expected to receive the GSK vaccine in the coming years in small amounts.
Only roughly 15 million doses can be produced annually, according to GSK. The Oxford vaccine might be produced in as many as 200 million doses annually, according to the Serum Institute.
Emeritus Liverpool School of Tropical Medicine professor Alister Craig advised nations attempting to obtain the GSK vaccination to switch to the Oxford vaccine instead.
In a few years, the number of severe illnesses and fatalities brought on by malaria could be drastically reduced, according to Craig, if the new vaccine is widely distributed throughout Africa.
Both malaria vaccines do not stop transmission, thus immunization programs by themselves will not be sufficient to stop epidemics. The proliferation of invading mosquito species and the rising reports of drug resistance to the primary treatments for malaria are further complicating efforts to stop the illness.
You would be mistaken to believe that this vaccination will put a stop to the malaria epidemic, said Craig.
Separately, the WHO expert group approved the Takeda dengue vaccine, which had previously received approval from the European Union’s pharmaceuticals agency.